The force that blood being pumped out by the heart is exerting on the major blood vessels and arteries, that move oxygenated blood to different parts of the body is known as Blood Pressure (BP).
Hypertension, also known as High Blood Pressure (HBP) or elevated blood pressure is an abnormal increase in this pressure.1,2
This disease is a major cause of premature death globally, because it commonly does not present with any symptoms at the early stage; hence the first symptom might just be a severe complication such as stroke, which could kill the patient instantly.
For this reason, hypertension is also tagged a “silent killer.” Stroke occurs when blood supply to the brain is affected as a result of a block, or rupture of a blood vessel leading to bleeding inside the brain.2
In this article, we will discuss everything you need to know about hypertension, including its risk factors, symptoms, types and stages, diagnosis, prevention, treatment, complications, and the various myths about hypertension.
Interesting Facts About Hypertension
In 2021, about 1.28 billion adults aged 30 – 70 years were diagnosed with hypertension globally, with most (about two-thirds) living in low- and middle-income countries. It is estimated that about half of people with hypertension are not aware that they have the disease.2
It is further estimated that 1 in 4 men, and 1 in 5 women have hypertension.3 Hypertension has been found to be more common in urban than rural communities, and that rural diet offers some form of protection against hypertension.4
Blood pressure is recorded in two numbers, one on top and one under. The one on top is known as the systolic blood pressure, and is the pressure exerted on the arteries when the heart contracts to push out blood; while the one under is the diastolic blood pressure, which is the pressure recorded when the heart muscles relax.
Normal blood pressure reading is 120/80mmHg or less, but usually not lower than 90/60mmHg. Very low blood pressure is termed hypotension, and could be a medical emergency.
Some persons, who are on antihypertensive medication, and not monitoring their blood pressure properly, may eventually reduce the blood so low, and can result in the person’s death.
Blood pressure measurement of 140/90mmHg and above, after at least two consecutive days measurements is considered hypertension.2,5 World health Organization Study Group recommended sitting position for recording blood pressure.6
Risk Factors for Hypertension1-6

Lifestyles, situations and behaviours that predispose individuals to having hypertension disease, are known as risk factors for the disease.
There are some risk factors that individuals can voluntarily avoid, in order to prevent them from getting hypertension disease. These are known as modifiable risk factors, while those that individuals cannot voluntarily avoid, are called non-modifiable risk factors
Non-Modifiable Risk Factors
- Family history: It has been found out that persons whose parents, siblings, or close relatives have hypertension, are more prone to develop the disease
- Race: Hypertension has been found to occur more in blacks than whites. The highest burden of the disease is found in Sub-Saharan African region
- Age: the disease occurs more in the older age group, especially from 65 years of age. This usually is as a result of progressive narrowing of the lumen of the arteries through which the heart pumps blood, thus increasing the force needed to get blood moving through those vessels. This narrowing could be as a result of fat deposits inside the lumen of the blood vessels
- Sex: Hypertension occurs more in males than females. It affects 1 in 4 males, while 1 in 5 females are affected
Modifiable Risk Factors
These factors are largely related to the individual’s lifestyles, and include;
- Unhealthy diet: Persistent consumption of diet rich in saturated fat such as red meat and high fat dairy foods (e.g., whole milk, ice cream, butter, cheese) predisposes one to developing hypertension. Inadequate consumption of diet rich in vegetables, fruits and potassium micronutrient is also a risk factor for developing hypertension.
- Increased salt intake: Cooking salt is sodium chloride. The sodium component has been found to contribute to development of hypertension.
- High Cholesterol level in the blood: This eventually leads to deposition of cholesterol on the lining of the lumen of blood vessels, thus narrowing them; and making it more difficult for blood to be pumped through them.
- Diabetes Mellitus: It has been found that many people, who have diabetes mellitus disease, eventually develop hypertension. Such persons are advised to monitor their blood pressure closely.
- Excessive alcohol consumption: Increased alcohol consumption increases ones chances of developing hypertension.
- Tobacco smoking: Smoking tobacco, in addition to being risk factor for many cancers is also a significant risk factor for developing hypertension.
- Overweight and Obesity: These commonly result from excessive consumption of unhealthy food, and reduced physical activity. Overweight occurs when the body mass index (BMI) of the individual is above 25kg/m2, but less than 30kg/m2. BMI values that are above 30kg/m2 is obesity
- Poor physical activity: It is recommended that adults do physical exercises for a total of two and half hour’s period every week. This could be conducted for thirty minutes every day, for five days in a week.
- Stress: This is emotional and physical disturbance commonly related to pressure of daily life activities and uncertainties associated with good living standards.
Symptoms of Hypertension2,3
Hypertension may not present with any symptom before a severe complication appears, hence it is also known as “silent killer”. It is important that every adult checks his/her blood pressure regularly. When symptoms occur, they include;
- Blurring of vision
- Noise in the ears
- Nose bleeding
- Early morning headaches
- Chest pain
- Irregular heartbeats
- Nausea
- Vomiting
- Confusion
Observed symptoms usually depend on the level of the raised blood pressure.
Types and Stages of Hypertension1,5,7,9
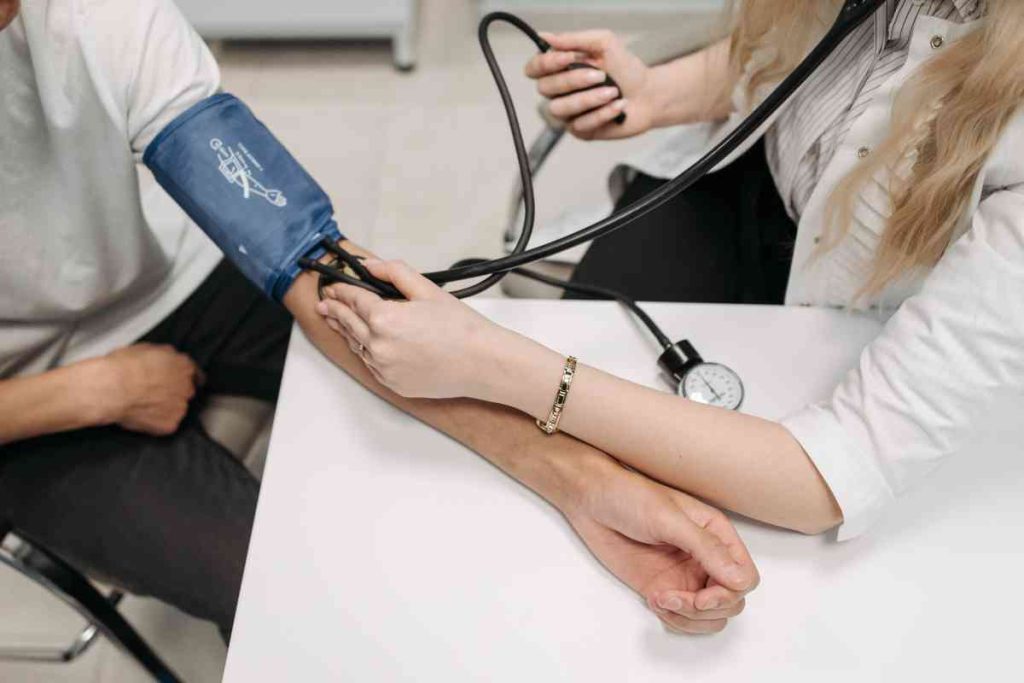
Types
Broadly, hypertension can be classified as primary or secondary hypertension.
Primary hypertension: This is also called Essential hypertension, and occurs in about 90% of cases. In this type of hypertension, no clear cause is found, with the disease commonly attributed to lifestyle, environmental, and genetic factors.
Secondary hypertension: This accounts for about 10% of cases, and has an identifiable cause such as renal, cardiovascular, neurogenic, endocrine, diseases or drugs. In many cases, causes of secondary hypertension can be remedied and the patient’s blood pressure normalized.
Some rare forms of hypertension are classified as follows;
- Pregnancy induced hypertension: Blood pressure is only raised when the woman is pregnant. Normally, pregnancy induced hypertension is not associated with swelling of the feet of the woman and protein in the urine. When the legs are swollen, and there is protein in the urine, during the last trimester of pregnancy, then the woman has a health condition known as Pre-eclampsia. Pre-eclampsia is a worrisome obstetrics health condition that requires immediate intervention to bring the blood pressure down. If this is not successfully done, then the woman might progress to Eclampsia; a situation where seizure sets in. Eclampsia is life-threatening.
- Isolated systolic hypertension: In this situation, only the systolic blood pressure is raised above 140mmHg while the diastolic blood pressure is not above 90mmHg. It is commoner in people aged 60 years and above, and thought to be due to hardening of arteries with age.
- White coat hypertension: In some individuals, the blood pressure may temporally rise when they visit a doctor for consultation, or at the mere sight of a Sphygmomanometer (instrument for measuring blood pressure). The blood pressure is normal when measured in other locations and possibly, by different health workers.
Stages of Hypertension
Previously, hypertension used to be categorized globally into four broad stages depending on the level of blood pressure recorded. The first stage was Mild hypertension, when the blood pressure is between 140/90mmHg to 160/100mmHg.
The second stage was Moderate hypertension, when the blood pressure is between 160/100mmHg to 180/110mmHg. In Severe hypertension, the diastolic blood pressure is between 110mm Hg to 120mm Hg. Diastolic blood pressure readings above 120mmHg is said to be Malignant hypertension.
However, in 2014, the American Joint National Committee on hypertension (JNC-VI) gave a classification which is mostly used globally for clinical and epidemiological purposes. The classification is;
- Optimal: Blood pressure that is less than 120/80mmHg, but above 90/60mmHg
- Normal: Systolic blood pressure of 120 – 129mmHg, and diastolic of 80 – 84mmHg
- High Normal: Systolic blood pressure of 130 – 139mmHg, and diastolic of 85 – 89mmHg
- Stage 1 (mild): Systolic blood pressure of 140 – 159mmHg, and diastolic of 90 – 99mmHg
- Stage 2 (moderate): Systolic blood pressure of 160 – 179mmHg, and diastolic of 100 – 109mmHg
- Stage 3 (severe): Systolic blood pressure that is 180mmHg and above, and diastolic of 110 and above
- Hypertension Urgency: Systolic blood pressure above 180mmHg, and diastolic of 130mmHg and above; but no organ damage
- Hypertensive Emergency: Rapid increase in systolic blood pressure to 210mmHg and above, and diastolic of 130mmHg and above. This is usually associated with organ damage
In 2017, American College of Cardiology and American Heart Association (ACC/AHA) proposed another guideline that now categorizes hypertension into;
- Normal: When the blood pressure is less than120/80mmHg
- Elevated: Systolic blood pressure of 120 – 129mmHg, and diastolic less than 80mmHg
- Stage 1: Systolic blood pressure between 130 – 139mmHg, and diastolic between 80 – 89mmHg
- Stage 2: Systolic blood pressure of at least 140mmHg, and diastolic of at least 90mmHg
- Hypertensive crisis: This is systolic of 180mmHg and above, and/or diastolic of 120mmHg and above. This is usually an emergency.
Some countries have their own categorization in use. An example is the classification given by the Nigerian Hypertension Society, as shown below;
- Optimal: Blood pressure reading that is less than 120/80mmHg
- Normal: Systolic blood pressure that is less than 130mmHg, and diastolic that is less than 85mmHg
- High Normal: Systolic of 130 -139mmHg, and diastolic of 85 – 89mmHg
- Grade 1 (Mild): Systolic of 140 – 159mmHg, and diastolic of 90 – 99mmHg
- Grade 2 (Moderate): Systolic of 160 – 179mmHg, and diastolic of 100 – 109mmHg
- Grade 3 (Severe): Systolic of more than 180mmHg, and diastolic of more than 110mmHg
Diagnosis of Hypertension1,2,7,9,10,11
Diagnosis of hypertension usually starts with good history taking from the patient. The doctor asks question on any specific complaint from the patient, the duration and specific features associated with the complaint, past medical/surgical history, and family/social history.
General physical examination is conducted, including measurement of the blood pressure. Sphygmomanometer, also known as Blood Pressure (BP) monitor is the instrument used for recording BP and ultimately determining if an individual is hypertensive or not.
Two arms of an individual could give slightly different blood pressure readings. It is recommended that the two arms are used at first, and then the one with higher BP is now continuously used for BP monitoring.
In the past, readings that are consistently above 140/90mmHg used to be considered hypertension, but recently systolic blood pressure that is consistently higher than 130mm Hg, and/or diastolic that is consistently above 80mmHg is now considered hypertension.
The measurement has to be taken in at least two or three different occasions within one week, before a diagnosis of hypertension is made.
However, in cases of severe hypertension, the diagnosis can be made with about two readings taken with a reliable sphygmomanometer in one occasion. The person measuring the BP has to be one that is properly trained, and the instrument should be reliable and in good working condition.
Certain basic investigations are done to determine if there is possible cause(s) of the disease and/or to assess the extent of complications associated with the disease if any. Some of these investigations are;
- Urinalysis: This urine test reveals if there is protein, blood or glucose in the urine. Presence of protein or blood could point to kidney disease, while presence of sugar is an indication that the patient possibly also has diabetes mellitus
- Blood Electrolyte, Urea and Creatinine: This laboratory investigation is also called Kidney Function Test, since derangement of the results is an indication of malfunctioning of the kidneys
- Lipid Profile assessment: Blood sample is tested in the laboratory, to determine the levels of lipids in the blood. Above normal levels of Cholesterol and Low-Density Lipoprotein (LDL) could imply that the patient might develop complications such as stroke or myocardial infection
- Thyroid function Test: High levels of the different components of this test could lead to increased blood pressure and pulse rate (increased heart beat). These high levels indicate a disease entity known as Thyrotoxicosis. Hypertension resulting from thyrotoxicosis is secondary hypertension, and usually resolves if the primary health condition is addressed
- Chest X-ray: Chest X-ray gives important information such as size of the heart, unfolding of aorta (the major blood vessel that pumps oxygenated blood out of the heart), fluid in the lungs, etc. Enlargement of the heart, unfolding of the aorta, and fluid in the lungs are all indications that heart failure complication has set in.
- Electrocardiogram (ECG): This test is used to assess the electrical activity of the heart. It helps in the diagnosis of heart disease, which could be a complication of hypertension.
- Echocardiogram: Ultrasound waves are used to display the action of the heart as it beats, with the aim of investigating and making diagnosis of heart diseases. It provides more information than ECG. Also used in assessing the effect of hypertension on the heart.
- Abdominal Ultrasound: Plain abdominal ultrasound could also be done to check the state of the kidneys. Pre-existing kidney pathology could lead to secondary hypertension, while hypertension that had lasted for a long time could cause injury to the kidneys
Prevention of Hypertension 2,10,11,12,13,14
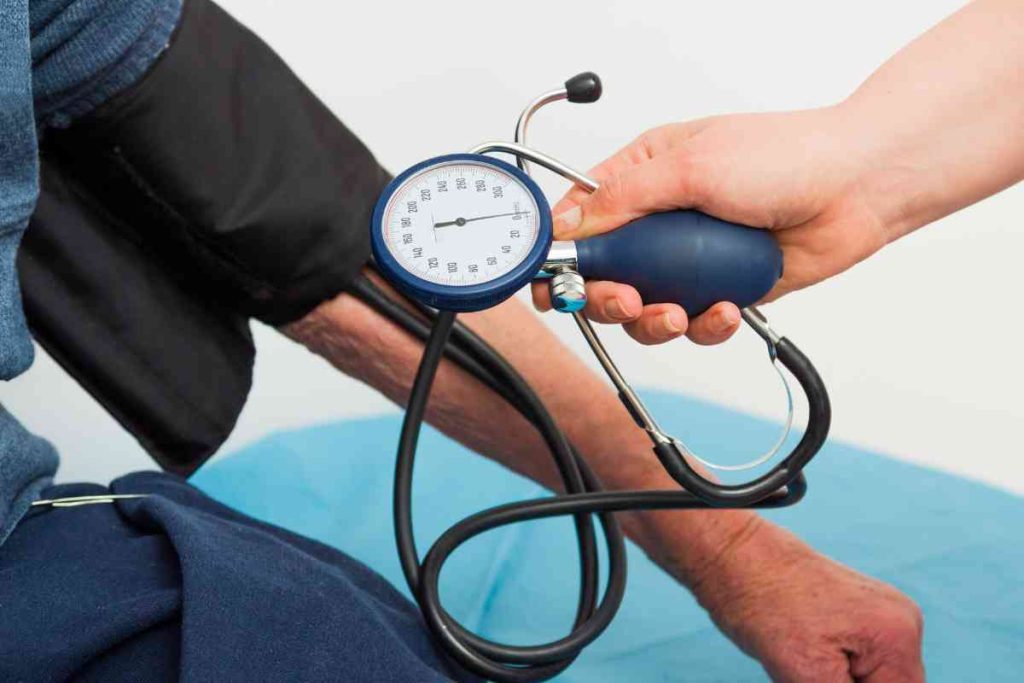
Primary prevention of hypertension aims at ensuring that people are not afflicted with the disease. The strategies essentially involve adopting healthy lifestyles, and ensuring that those modifiable risk factors are avoided. It also seeks to create enough awareness among those with non-modifiabl risk factors, about the need to keep an eye on their blood pressure. The specific preventive steps used to avoid those risk factors are;
- Consumption of healthy diet: One should avoid consumption of diet rich in saturated fat such as red meat and high fat dairy foods. Dietary Approach to Stop Hypertension (DASH) diet recommended by the U.S. National Heart, Lung, and Blood Institute (NHLBI); has been found very useful in preventing hypertension. DASH diet contains vegetables, fruits, lean protein, whole grains, legumes, nuts, and low fat dairy products. This DASH diet also provides the required potassium intake, which also assists in preventing hypertension
- Avoidance of excessive salt intake: Cooking salt is sodium chloride. The sodium component has been found to contribute to development of hypertension. It is advised that people reduce their salt intake and avoid adding salt to already prepared meal. It is also very important to avoid salty processed food.
- Avoidance of excessive consumption of cholesterol-rich diet: This prevents deposition of cholesterol on the lining of the lumen of blood vessels, thus avoiding narrowing of the lumen, which could lead to increased blood pressure. Food rich in cholesterol include eggs, cheese, sardines, full fat yogurt, processed meat such as hot dogs and sausages, cake and ice cream.
- Proper management of Diabetes Mellitus, and regular blood pressure check for diabetic patients: Since diabetes mellitus is a risk factor for developing hypertension, adequate control of blood sugar helps in reducing the chances of the diabetic patient developing hypertension. Regular monitoring of the blood pressure is also advised.
- Avoidance of excessive consumption of alcohol: Increased alcohol consumption increases ones chances of developing hypertension; hence reducing the quantity of alcohol consumed, helps in preventing hypertension.
- Avoidance of Tobacco smoking: Complete avoidance of tobacco smoking is very beneficial in preventing development of hypertension.
- Not being overweight or Obese: Taking healthy diet, and regular exercises assist in maintaining recommended body weight. Not being overweight or obese contribute in preventing hypertension
- Being physically active: It is recommended that everybody engages in at least 150 minutes of exercises every week. Aerobic exercises are preferable. This translates to 30 minutes of moderated exercises every five days of the week. Some of the exercises that can be used are; walking, jogging, cycling, swimming, dancing, etc. It is advised that duration and intensity of exercises be increased gradually before getting to the recommended duration of 150 minutes in a week People who live sedentary life are more prone to developing hypertension than those who live active and mobile life.
- Avoidance of stressful situations: It is nice to avoid, as much as is possible; situations that lead to anger, conflicts, fights and such events that generate intense harmful emotions, since these are known to lead to hypertension, especially when they are reasonable parts of one’s everyday life. Rest, good sleep, and some relaxation/recreational activities such as listening to music, dancing, meditation, yoga, etc also reduce stress.
Specifically, primary level hypertension prevention entails health promotion activities such as health education and awareness creation programmes through print, electronic or social media. These are strategies that can be used to inform and educate people on the need to modify their lifestyle, with the ultimate aim of preventing hypertension.
The secondary level Hypertension prevention is early diagnosis and treatment of the disease, which enhances reduction in the morbidity and mortality associated with the disease. Diagnosis of hypertension is easily made by correctly checking the blood pressure a couple of times with good sphygmomanometer.
Routine screening of blood pressure for all patients that visit any health facility and community blood pressure screening outreach activities are very useful in making early diagnosis of hypertension.
Tertiary level hypertension prevention deals with limitation of disability arising from the disease, and rehabilitation of those patients that sustained disabling complications as a result of the disease. Inability to use the limbs, as a result of stroke is an example of such complications that require rehabilitation. Efforts are made to get the patient regain the use of the limbs, as much as is possible.
How to Treat Hypertension3,15,16
Treatment of hypertension should usually commence with reduction in the modifiable risk factors that have been associated with the patient. In some cases, these steps result in reasonable reduction of the blood pressure.
There are however, different classes of drugs available for treatment of hypertension. These drugs lower blood pressure by exerting action on different parts of the body, and in different ways. The classes of the commonly used ones are;
- Calcium-channel antagonist
- Diuretics
- Angiotensin Converting Enzyme (ACE) inhibitors
- Angiotensin II receptor antagonists
- Beta-blockers
- Centrally acting drugs
- Vasodilators
It is extremely important that any patient that has hypertension should be completely managed by a qualified medical doctor. Inappropriate use of antihypertensive drugs led to the death of some hypertensive patients.
Some patients continuously take drugs without adequately monitoring their blood pressure. This has resulted in the blood pressure being so low (hypotension) and eventually leading to fatal outcomes.
Complications of Hypertension1,2,4,9,11,17-20

Hypertension is said to be the number one risk factor for death in the world. This, it does by inflicting severe complications on certain vital organs of the body such as brain, heart and blood vessels, kidneys, and eyes.
Hypertension that is undiagnosed and treatment not commenced early, gradually damages these vital organs of the body. Effects on these organs could lead to the following complications;
Brain
Untreated or poorly treated hypertension could result in rupture or blockage of a blood vessel in the brain. This sudden interruption of blood supply to the brain leads to loss of brain function, a condition known as “stroke”.
Stroke is the third leading cause of death in North America. The manifestation of stroke depends on the usual functions of the areas of the brain that the blood supply was interrupted. Common manifestations of stroke include; impaired use of the limbs and impaired speech.
The extent of manifestation depends on the site, and extent of rupture or blockage. Severe bleeding into the brain could cause unconsciousness or even immediate death. Stroke is the commonest complication of hypertension.
Stroke is said to be haemorrhagic when it is as a result of rupture of a blood vessel, and ischaemic/thrombotic when it is as a result of blockage of a blood vessel.
In addition to rupture or blockage of the blood vessel in the brain, gradual reduction in the lumen of the blood vessels in the brain, leading to sustained diminishing of blood supply to the brain, could play a role in memory decline and development of dementia.
Cardiovascular system
The heart and blood vessels that move blood around the body and the lungs make up the circulatory system.
The network of blood vessels that transport blood all over the body, except the lungs is call the systemic blood circulation; while the network of vessels that transport blood to the lungs for oxygenation of the blood, and back to the heart is known as pulmonary circulation.
As a result of the added pressure needed to pump blood by the heart in cases of hypertension, the heart later gets weak and enlarged with time.
The high-pressure impact on the arteries in hypertensive patients could lead to cracks on internal walls of the arteries, allowing for deposition of cholesterol inside those cracks; and ultimately leading to formation of plaques that narrow the vessels.
These narrowing compromises blood flow through the vessels. The high blood pressure could also lead to thinning of the vessels, which could manifest as a bulge; and later rupture, causing internal bleeding.
The bulge could also press on a vital organ leading to some complications. This effect of hypertension on the circulatory system is progressive, leading to complications, if the blood pressure is not controlled.
It has been documented that about 60% of cardiovascular diseases globally are due to hypertension, and about 80% of cardiovascular deaths occur in low- and middle-income countries.
These complications include;
- Heart Attack: In this, blood supply to the heart is compromised, and that portion of the heart which blood supply is diminished or blocked is deprived of oxygen and essential nutrients. Heart Attack could present as severe chest pain and irregular heartbeat, and lead to sudden death.
- Heart Failure: As a result of continued utilization of high pressure in trying to pump blood against increasing resistance, the heart eventually gets weaker and weaker, and ultimately becomes ineffective in adequately pushing blood from the heart, to the other parts of the body. This is called heart failure. It commonly manifests as the patient becoming unduly weak after a little exertion, swelling of the feet, discomfort when lying down flat, and cough.
- Aneurysm: The high pressure with which the heart pumps blood against the walls of the blood vessels, eventually leads to cracks and weakening of some portions of the vessels; which ultimately results in bulging or ballooning of those section, known as aneurysm. The aneurysm can easily rupture, resulting in internal bleeding into the areas where it is located. Clinical picture following rupture of an aneurysm depends on the location and size of the aneurysm. Rupture of aneurysm of the aorta, which is the major blood vessel carrying blood out of the heart, could result in death within minutes; while rupture of a very small aneurysm in the brain might present as a treatable stroke.
- Angina Pectoris: It is chest pain that usually occurs when the demand for blood supply to the heart exceeds the supply. This is as a result of blockage of the coronary artery that supplies blood to the heart. The pain commonly manifests during exercises, and could radiate to the jaw and arms.
- Irregular heartbeat: The sustained strain on the heart as a result of uncontrolled blood pressure could result in the heart beating irregularly. Irregular heartbeat is a cause of heart attack.
- Pulmonary embolism: Pulmonary hypertension occurs when there is raised blood pressure in the pulmonary circulation; that is blood supply to the lungs. The high blood pressure as seen in systemic hypertension also could lead to cracks and deposition of cholesterol and lipids inside the pulmonary blood vessels. The arterial plaques formed could block blood flow to a section of the lungs, a condition known as pulmonary embolism. In severe cases, the condition could lead to death.
Kidneys
When uncontrolled hypertension leads to blockage or rupture of blood vessels that supply the kidneys, it causes damage to the affected sections of the kidneys, and ultimately diminishes it’s functionality.
If unchecked, this process eventually progresses to chronic kidney failure, and possibly other kidney complications.
Eyes
The effects of uncontrolled blood pressure on the eyes also lead to blockage and rupture of the tiny blood vessels in the eyes. These particularly affect the retina, leading to eye findings called retinopathies. These could present as blurring of vision, eye ache, or even blindness.
Myths and Misconceptions about Hypertension21-23
There are some commonly held false beliefs and notions about hypertension. These have reasonably contributed to morbidity and mortality associated with hypertension. Consequently, it is crucial that correct information on these misconceptions is provided. The misconceptions include;
I. Symptoms and signs of hypertension are usually obvious
This is certainly not correct. Hypertension is tagged “Silent killer” because in many cases, severe complication is the first sign to the patient that he/she is unhealthy.
II. Hypertension affects only old adults
Hypertension also affects adolescents and children. Obese adolescents and children are at risk of developing hypertension. Their blood pressure should also be regularly checked. Secondary hypertension can occur in them as a result of endocrine, renal, neurogenic, cardiac/vascular diseases or drug induced.
III. As long as I do not add salt to my already prepared regular meal, I will not have hypertension.
Certainly not true. Some deliberately add too much salt in their meal during preparation, and believe that the problem is with “uncooked” salt. Some also indulge in consumption of excessively salted prepared snack food such as potato chips, pizza, cheeseburger, sandwiches, meat dishes, etc.
IV. Since hypertension runs in my family, I need not work towards preventing it, because I must eventually get it.
This assertion is not correct. Though positive family history of hypertension is a non-modifiable risk factor for developing the disease, taking determined steps to ensure that the person at risk does not develop the disease in most cases, achieves the desired results. Some of these recommended steps include; eating healthy diet, being physically active, not smoking, avoiding excessive consumption of alcohol, avoiding stressful situations, and very importantly monitoring the blood pressure closely.
V. If on antihypertensive drugs, and my blood pressure check records normal reading, then I am cured and should stop taking any more antihypertensive medication.
Hypertensive patients should not regulate use of antihypertensive medication on their own. They should always comply with the recommendations of their attending Physician. Initial use of drugs in most cases could bring the blood pressure reading to normal value. This however, usually rises again once the medication is completely stopped. The Physician usually keeps adjusting the drugs and dosages until adequate control of the blood pressure is achieved. Improper use of the drugs could also result in the blood pressure becoming very low (hypotension), which could lead to fatal outcomes. In cases of secondary hypertension where the cause of the disease is known, effective treatment of the cause; commonly results in remission of the high blood pressure. The decision on this should usually be left to the attending Physicians.
VI. Since it is said that red wine is good for the heart, then I can take as much quantity of red wine as I desire, even if I am hypertensive.
Red wine contains reasonable quantity of alcohol, which is the item that is implicated as a risk factor in causation of hypertension. That the alcohol is now inside red wine does not make it harmless. One should always refrain from consuming excessive quantity of alcohol.
VII. Sexual intercourse increases the risk of developing hypertension.
Sexual intercourse is a form of exercise, hence contributes to the physical activity of those engaged in it. It is rather beneficial in preventing hypertension. It can only be harmful if the individual already has existing illness, especially cardiac illness.
VIII. Alternative medical practitioners treat hypertension and stroke better than orthodox medical practitioners.
This misconception has led to the death of many hypertensive and stroke patients, especially in the low- and middle-income countries. Medical science has made so much progress in the area of treating hypertension and stroke. So many effective drugs are now available, and also health workers are sufficiently trained to manage hypertension and stroke.
IX. Giving injection to any patient that has hypertension or stroke, invariably leads to worsening of the problem and even fatal outcome.
This certainly is not true. Some injections are life-saving for some hypertensive and stroke patients. The decision to use injections in treating hypertensive or stroke should be left to the Physician.
X. Stroke is better managed in prayer houses.
So many persons in low- and middle-income countries believe that stroke is usually an evil attack from some perceived enemies. Hence, they are convinced that it is only direct divine intervention that can heal the patient. Consequently, the patient is taken to prayer/spiritual house for healing. Some patients die in that process before they are rescued. Stroke is a pure medical condition, and is effectively managed by trained medical personnel.
XI. Once the body of a patient who has stroke touches the ground, then the patient must die.
This false belief is again reasonably common in some low- and middle-income countries. The outcome of the management of a patient who has stroke is not determined by the patient’s body touching the ground or not. Patients who have stroke can safely lie down on the ground while waiting for transportation to the hospital, if that is the only comfortable thing to do.
XII. Hypertension is caused by evil curse placed on the victim
A curse is not a known risk factor for hypertension. Believing that evil curses can result in hypertension is one of the reasons people take their hypertensive patients to prayer houses and alternative medical practice outfits. There are scientifically proven risk factors for hypertension.
XIII. I do not think too much, hence I cannot develop hypertension.
Stress that arises from excessive thinking and worrying is not the only risk factor for developing hypertension. Even if one does not think too much, he/she could be in danger of developing hypertension as a result of exposure to the other risk factors.
XIV. I am a jolly good fellow, hence I cannot develop hypertension
Being frequently happy does not guarantee that one will not develop hypertension. As stated earlier, other risk factors could play roles in one developing hypertension.
MESSAGE from Community Positive Health Attitude Initiative Team
Hypertension is ravaging mankind. Globally, the number of people aged 30 to 79 years with the disease has doubled between 1990 and 2019.24 We love you, and your family/friends love you too. You still have so much to contribute to the wellbeing of your loved ones and humanity generally.
This disease can be effectively managed and controlled if detected early. Remember; hypertension is a SILENT KILLER! Please check your blood pressure, and comply with the recommended follow-up steps, if it is high.
Do not say “IT IS NOT MY PORTION.” It certainly can be anyone’s portion!
REFERENCES
- Obionu CN. Guide to Tropical Public Health and Community Medicine. First Edition, EZU BOOKS LTD, Enugu, Nigeria, 2018.
- World Health Organization. https://www.who.int/news-room/fact-sheets/detail/hypertension (Accessed, 27/10/2022)
- World Health Organization. https://www.who.int/health-topics/hypertension (Accessed, 27/10/2022)
- Ogunmekan DA, Osibogun AO, Seedat YK, Onajole AT. Public Health in Africa. Centre for Epidemiology and Health Development, University of Lagos, Nigeria. 2018
- Food and Drugs Administration. https://www.fda.gov/drugs/special-features/high-blood-pressure-understanding-silent-killer#:~:text=Why%20is%20it%20important%20to,and%20stroke%2C%20among%20other%20things. (Accessed, 27/10/2022)
- World Health Organization. Bull World Health Organization, Vol 61(1) 53; 1983
- Medscape. https://emedicine.medscape.com/article/241381-overview#:~:text=Normal%3A%20Systolic%20lower%20than%20120,100%20mm%20Hg%20or%20greater (Accessed, 27/10/2022)
- Whelton PK, Carey RM, Aronow WS, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol 2018;71:e127–e248. [PubMed: 29146535]
- Healthline. https://www.healthline.com/health/high-blood-pressure-hypertension/how-reduce-high-blood-pressure#talk-to-your-doctor (Accessed, 27/10/2022)
- https://www.hopkinsmedicine.org/health/conditions-and-diseases/high-blood-pressure-hypertension/high-blood-pressure-prevention-treatment-and-research (Accessed, 23/11/2022)
- Medical News Today. https://www.medicalnewstoday.com/articles/150109#summary (Accessed, 23/11/2022)
- CDC. https://www.cdc.gov/bloodpressure/prevent.htm (Accessed, 25/11/2022)
- NHS. https://www.nhs.uk/conditions/high-blood-pressure-hypertension/prevention/ (Accessed, 25/11/2022)
- Appel LJ, Moore TJ, Obarzanek E, et al.; DASH Collaborative Research Group. A clinical trial of the effects of dietary patterns on blood pressure. N Engl J Med 1997;336:1117–24. [PubMed: 9099655]
- Falase AO, Akinkugbe OO. A Compendium of Clinical Medicine. New Edition, 2007. Spectrum Books Ltd, Ibadan, Nigeria.
- Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/high-blood-pressure/diagnosis-treatment/drc-20373417 (Accessed, 25/11/2022)
- World Heart Foundation. https://world-heart-federation.org/resource/infographic-hypertension-nutrition/ (Accessed, 25/11/2022)
- Forouzanfar MH, Liu P, Roth GA, et al. Global burden of hypertension and systolic blood pressure of at least 110 to 115 mm Hg, 1990–2015. JAMA 2017;317:165–82. [PubMed: 28097354]
- GBD 2016 Risk Factors Collaborators. Global, regional, and national comparative risk assessment of 84 behavioural, environmental and occupational, and metabolic risks or clusters of risks, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet 2016;390:1345–422.
- World Health Organization. Cardiovascular Disease: Prevention and Control. WHO Report 2007. WHO, Geneva, Switzerland
- https://www.keckmedicine.org/blog/10-blood-pressure-myths-and-facts/ (Accessed, 25/11/2022)
- https://www.heart.org/en/health-topics/high-blood-pressure/the-facts-about-high-blood-pressure/common-high-blood-pressure-myths (Accessed, 25/11/2022)
- Oke DA, Bandele EO. Misconceptions of Hypertension. Journal of the National Medical Association, 2004, 96 (9): 1221 – 1224
- NCD Risk Factor Collaboration (NCD-RisC)* Lancet2021; 398(10304): 957–80. https://www.thelancet.com/article/S0140-6736(21)01330-1/fulltext
